
Anxiety Symptoms: Signs, Causes and When to Seek Help
Last updated:
By Senior Medical Writer | Reviewed for Clinical Accuracy | Last Updated: February 2026
TL;DR: Executive Summary
- Core Definition: Anxiety is a natural survival mechanism, but it becomes clinical when it is disproportionate, persistent, and interferes with daily life (NICE Guidelines).
- Physical Impact: Manifests through ‘Somatic Mapping’—affecting the heart, gut, and nervous system via the Vagus Nerve.
- Biological Root: Driven by the ‘Amygdala Hijack’ and elevated Cortisol levels.
- The Red Flag Rule: Seek professional help if your GAD-7 score is 8 or higher, or if symptoms persist for more than two weeks.
- UK Pathway: Access support via your GP or self-refer to NHS Talking Therapies.
Introduction: Understanding the Spectrum of Anxiety
Anxiety is not merely a ‘feeling’; it is a sophisticated biological programme designed to ensure human survival. In the United Kingdom, anxiety disorders represent the most common mental health condition, affecting approximately 1 in 6 adults in any given week (NHS Digital). While acute anxiety serves as a vital alert system, chronic activation of this state leads to systemic physiological and psychological exhaustion.
Claim: Clinical anxiety is distinguished from ‘normal’ stress by its duration and the absence of an immediate external threat. Evidence: The National Institute for Health and Care Excellence (NICE) defines Generalised Anxiety Disorder (GAD) as excessive worry about a range of different events or activities on more days than not for at least six months. Source: NICE Clinical Guideline [CG113].
Biological Mechanisms: The Anatomy of the ‘Amygdala Hijack’
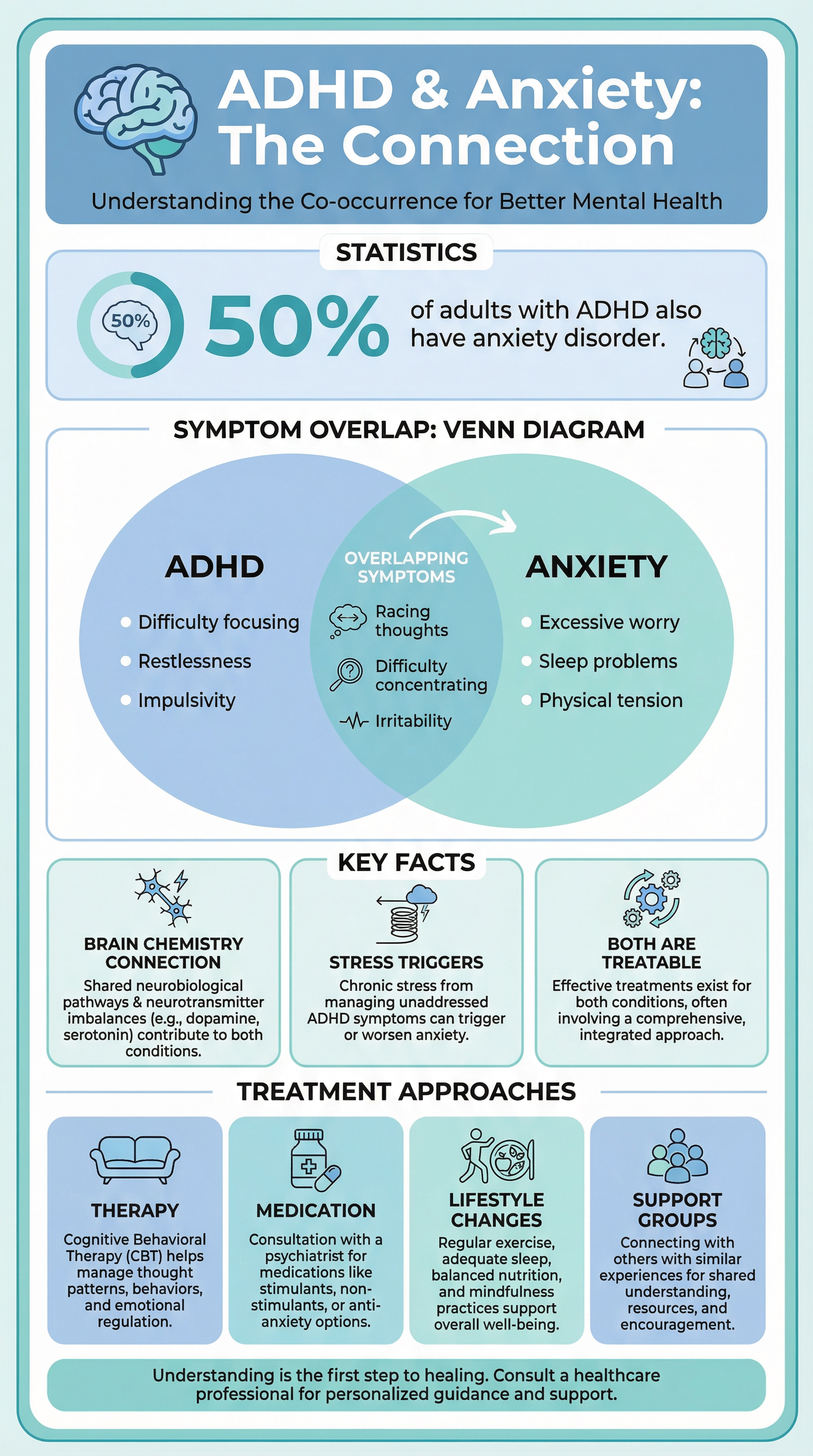
To understand anxiety symptoms, one must first understand the neurological ‘hardware’ that generates them. The process is governed by the Autonomic Nervous System (ANS), specifically the balance between the Sympathetic Nervous System (SNS) and the Parasympathetic Nervous System (PNS).
The Amygdala and Cortisol
The amygdala acts as the brain’s smoke detector. When it perceives a threat—real or imagined—it triggers the ‘Amygdala Hijack’, bypassing the rational prefrontal cortex. This stimulates the adrenal glands to release Cortisol and Adrenaline. Cortisol, the primary stress hormone, increases glucose in the bloodstream and alters immune system responses to prepare the body for immediate action.
The Vagus Nerve and Vagal Tone
The Vagus Nerve is the primary component of the Parasympathetic Nervous System. It serves as a bidirectional ‘superhighway’ between the brain and the internal organs. High ‘Vagal Tone’ allows the body to recover quickly after a stress response. Conversely, low vagal tone is associated with chronic anxiety, as the body struggles to exit the ‘fight-or-flight’ state and re-enter ‘rest-and-digest’.
Claim: Stimulating the Vagus Nerve can actively reduce anxiety symptoms by lowering heart rate and cortisol levels. Evidence: Research published in Frontiers in Psychiatry indicates that Vagus Nerve Stimulation (VNS) modulates the neural circuits involved in anxiety and depression. Source: PubMed (PMID: 29740354).
Granular Somatic Mapping: How Anxiety Manifests Physically
Anxiety is a whole-body experience. Patients often present with physical complaints long before they recognise the psychological root. This ‘somatic mapping’ categorises symptoms by physiological system.
| System | Common Symptoms | Biological Driver |
|---|---|---|
| Cardiovascular | Palpitations, chest tightness, tachycardia. | Adrenaline-induced heart rate acceleration. |
| Gastrointestinal (GI) | Nausea, IBS, ‘butterflies’, acid reflux. | Blood diversion from gut to skeletal muscles. |
| Neurological | Dizziness, ‘brain zaps’, tinnitus, paresthesia. | Hyperventilation and nervous system hyper-excitability. |
| Musculoskeletal | Bruxism (jaw clenching), tension headaches, back pain. | Chronic muscle guarding/bracing. |
Cardiovascular and Respiratory Signs
During an anxiety episode, the heart pumps faster to distribute oxygenated blood. This often leads to ‘air hunger’ or dyspnoea. Many individuals mistake these symptoms for a cardiac event, which further exacerbates the anxiety—a phenomenon known as the ‘anxiety-panic cycle’.
The Gut-Brain Axis
The GI tract is often called the ‘second brain’ due to the Enteric Nervous System. Anxiety disrupts the microbiome and slows digestion, leading to chronic conditions like Irritable Bowel Syndrome (IBS). The NHS recognises a strong correlation between mental health and digestive behaviour.
Cognitive and Emotional Symptoms
Beyond the physical, anxiety alters the way the brain processes information. This includes:
- Executive Dysfunction: Difficulty concentrating, ‘brain fog’, and indecisiveness.
- Intrusive Thoughts: Persistent, unwanted ‘what-if’ scenarios.
- Dissociation: Depersonalisation (feeling detached from oneself) or Derealisation (feeling the world is ‘unreal’).
Claim: Chronic anxiety leads to structural changes in the brain, specifically shrinking the hippocampus. Evidence: Longitudinal studies show that prolonged exposure to high cortisol levels can reduce the volume of the hippocampus, which is responsible for memory and emotional regulation. Source: PubMed (PMID: 22403421).
Causes and Triggers: Why Does Anxiety Occur?
Anxiety is rarely caused by a single factor. It is typically a combination of:
- Genetics: A family history of mental health conditions.
- Environmental Stressors: Work pressure, financial instability, or relationship breakdown.
- Medical Mimics: Certain physical conditions can mimic anxiety symptoms, such as hyperthyroidism, Vitamin B12 deficiency, or cardiac arrhythmias. It is essential to rule these out via blood tests.
When to Seek Help: The GAD-7 Scale and Clinical Pathways
In the UK, the primary tool for assessing anxiety is the GAD-7 (Generalised Anxiety Disorder 7-item scale). This questionnaire asks patients to rate the frequency of their symptoms over the last two weeks.
Interpreting Your GAD-7 Score
- 0-4: Minimal anxiety.
- 5-9: Mild anxiety (Monitoring and self-help recommended).
- 10-14: Moderate anxiety (Clinical intervention usually required).
- 15-21: Severe anxiety (Urgent clinical intervention).
The UK Treatment Pathway
The NHS follows a ‘Stepped Care’ model. Step 1 involves recognition and assessment. Step 2 includes low-intensity interventions like guided self-help. Step 3 involves high-intensity psychological interventions like Cognitive Behavioural Therapy (CBT) or medication (SSRIs).
You can access NHS Talking Therapies (formerly IAPT) without a GP referral in many parts of England. This programme provides evidence-based treatments for anxiety and depression.
Frequently Asked Questions (FAQ)
Is a panic attack dangerous?
While physically distressing, a panic attack is not life-threatening. It is the body’s ‘fight-or-flight’ system activating at the wrong time. Symptoms usually peak within 10 minutes.
Can anxiety cause physical pain?
Yes. Chronic muscle tension (guarding) can lead to genuine musculoskeletal pain, particularly in the neck, shoulders, and lower back.
What is the quickest way to calm the Vagus Nerve?
Techniques such as ‘Box Breathing’ (inhale 4, hold 4, exhale 4, hold 4) or ‘Extended Exhalation’ (exhaling for longer than you inhale) stimulate the Parasympathetic Nervous System and signal the brain to relax.
How do I know if it’s anxiety or a heart problem?
If you experience sudden chest pain that radiates to your arm or jaw, or if you have extreme shortness of breath, you must call 999 or visit A&E immediately. If tests are clear, anxiety is a likely cause.
References:
- NHS (2024). Anxiety, fear and panic. [online] Available at: https://www.nhs.uk/mental-health/feelings-symptoms-behaviours/feelings-and-symptoms/anxiety-fear-panic/
- NICE (2019). Generalised anxiety disorder and panic disorder in adults: management. Clinical Guideline [CG113].
- Frontiers in Psychiatry (2018). Vagus Nerve Stimulation, Depression, and Inflammation.
- Journal of Neuroscience (2012). Chronic Stress and Hippocampal Atrophy.
Frequently Asked Questions
Is a panic attack dangerous?
While physically distressing, a panic attack is not life-threatening. It is the body’s ‘fight-or-flight’ system activating at the wrong time. Symptoms usually peak within 10 minutes.
Can anxiety cause physical pain?
Yes. Chronic muscle tension (guarding) can lead to genuine musculoskeletal pain, particularly in the neck, shoulders, and lower back.
What is the quickest way to calm the Vagus Nerve?
Techniques such as ‘Box Breathing’ (inhale 4, hold 4, exhale 4, hold 4) or ‘Extended Exhalation’ (exhaling for longer than you inhale) stimulate the Parasympathetic Nervous System and signal the brain to relax.
How do I know if it’s anxiety or a heart problem?
If you experience sudden chest pain that radiates to your arm or jaw, or if you have extreme shortness of breath, you must call 999 or visit A&E immediately. If tests are clear, anxiety is a likely cause.
Related Articles

Anxiety Causes: What Triggers Anxiety and Why
What causes anxiety? Explore the triggers, risk factors and underlying reasons anxiety develops - and what you can do about it.
Anxiety Causes: Exploring the Roots of Worry and Fear
Anxiety Causes TL;DR Anxiety can stem from various factors, including genetics, brain chemistry, life experiences, and chronic stress. Understanding these causes is the first step towards...

Anxiety Symptoms: Signs, Causes and When to Seek Help
Recognise the signs of anxiety - physical, emotional and behavioural. Learn what causes anxiety and when to seek professional help.