Understanding Agoraphobia: Symptoms, Causes, and NHS Treatment Options in the UK
Last updated:
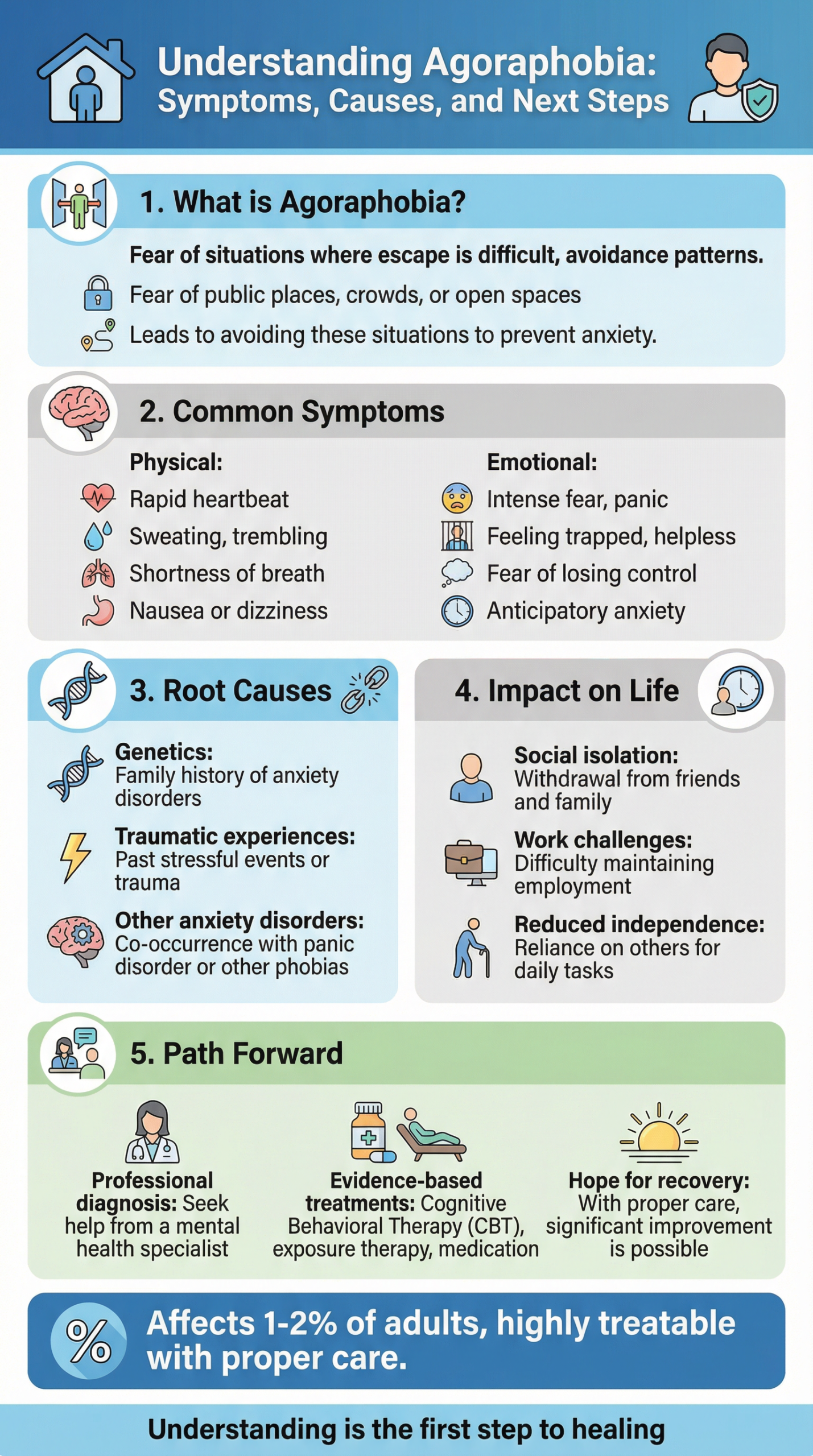
\n\nAgoraphobia is an anxiety disorder characterized by an intense fear of situations where escape might be difficult or help unavailable, often leading to significant lifestyle limitations. It commonly develops alongside panic disorder and involves complex interactions between physical, cognitive, and behavioral symptoms. This comprehensive guide explores the symptoms, causes, and treatment options available through the NHS in the UK.
What is Agoraphobia?

Agoraphobia goes beyond simple shyness or social anxiety. It’s a debilitating condition where individuals experience overwhelming fear in specific environments, particularly those perceived as unsafe or difficult to escape from. Common trigger situations include:
• Public transportation (buses, trains, planes) • Open spaces (parking lots, bridges, large fields) • Enclosed spaces (shops, theaters, small rooms) • Crowds or standing in line • Being outside the home alone
Symptoms of Agoraphobia
Physical Symptoms The physical manifestations of agoraphobia typically mirror panic attacks and occur when facing anxiety-provoking situations:
• Rapid heart rate and palpitations • Sweating and trembling • Nausea and stomach upset • Chest pain or tightness • Feeling faint or dizzy • Hyperventilation and shortness of breath • Tinnitus (ringing in ears)
Cognitive Symptoms The mental aspects involve persistent fears and catastrophic thinking patterns:
• Fear of embarrassment from visible panic attacks • Catastrophic thoughts about death or “losing control” • Worry about being trapped without help • Anticipatory anxiety about future situations • Dependency concerns about needing others for safety
Behavioral Patterns Agoraphobia significantly impacts daily behavior through avoidance strategies:
• Avoiding public transport, crowded spaces, or unfamiliar areas • Requiring a trusted companion to venture outside • Limiting activities to “safe” zones near home • In severe cases, becoming housebound for extended periods • Developing elaborate safety routines or escape plans
Causes and Risk Factors
Agoraphobia often develops as a complication of panic disorder, where recurrent panic attacks create anticipation of future episodes in specific environments. Contributing factors include:
Primary Causes • **Panic Disorder**: The most common precursor, with agoraphobia developing in response to repeated panic attacks • **Genetic Predisposition**: Family history of anxiety disorders increases risk • **Brain Chemistry**: Imbalances in neurotransmitters like serotonin and GABA
Environmental Triggers • Traumatic life events or significant stress • Major life transitions (moving, job loss, relationship changes) • Learned avoidance behaviors that reinforce fear cycles • Substance abuse or withdrawal
NHS Treatment Options
The NHS offers comprehensive, evidence-based treatments for agoraphobia, typically following a stepped care approach based on severity.
Psychological Therapies
**Cognitive Behavioral Therapy (CBT)** CBT is the gold standard treatment for agoraphobia, focusing on: • Identifying and challenging irrational fear-based thoughts • Gradual exposure to feared situations in a controlled manner • Developing coping strategies and relaxation techniques • Building confidence through successful experiences
*Example*: A patient might start by practicing short trips to local shops with therapist support, gradually increasing distance and complexity of journeys.
**Guided Self-Help** For mild to moderate cases, the NHS offers: • Structured self-help programs with workbooks • Online CBT modules and apps • Regular check-ins with mental health practitioners • Group therapy sessions for peer support
Medication Options

**First-Line Medications** • **SSRIs** (Selective Serotonin Reuptake Inhibitors): Sertraline, fluoxetine, or paroxetine are commonly prescribed to reduce anxiety symptoms • **SNRIs** (Serotonin-Norepinephrine Reuptake Inhibitors): Venlafaxine may be used as an alternative
**Alternative Medications** • **Pregabalin**: Prescribed for patients who cannot tolerate SSRIs • **Short-term Benzodiazepines**: Occasionally used for severe acute symptoms, but not recommended for long-term use due to dependency risks
Specialized Support Services
**Community Mental Health Teams (CMHT)** For severe cases, CMHTs provide: • Intensive outpatient support • Home visits when patients cannot travel • Crisis intervention services • Coordination with other healthcare providers
**Crisis Support** • NHS 111 for immediate mental health support • Local crisis helplines and emergency services • Samaritans (116 123) for emotional support
Accessing NHS Care
Step 1: GP Consultation • Book an appointment with your GP for initial assessment • Discuss symptoms, triggers, and impact on daily life • Receive referral to appropriate mental health services
Step 2: IAPT Services • **Improving Access to Psychological Therapies (IAPT)** services are available across the UK • Self-referral is possible in many areas for quicker access • Offers CBT, counseling, and group therapy options
Step 3: Specialist Services • For complex cases, referral to specialist anxiety clinics • Access to psychiatrists for medication management • Coordination with social services if needed
Treatment Outcomes and Recovery
With appropriate treatment, the prognosis for agoraphobia is generally positive:
• **CBT Success Rates**: 60-80% of patients show significant improvement • **Medication Effectiveness**: SSRIs help reduce symptoms in 70% of cases • **Combined Treatment**: The most effective approach often combines therapy and medication
Recovery Timeline • Initial improvement often seen within 6-12 weeks of starting treatment • Full recovery may take 6 months to 2 years depending on severity • Maintenance strategies help prevent relapse
Self-Help Strategies
While professional treatment is essential, several self-help techniques can support recovery:
• **Breathing Exercises**: Deep breathing techniques to manage panic symptoms • **Progressive Muscle Relaxation**: Systematic tension and release of muscle groups • **Mindfulness and Meditation**: Present-moment awareness to reduce anticipatory anxiety • **Gradual Exposure**: Slowly increasing exposure to feared situations at your own pace • **Support Networks**: Connecting with family, friends, or support groups
Living with Agoraphobia
Recovery from agoraphobia is possible with the right support and treatment. The NHS provides comprehensive services designed to help individuals regain their independence and quality of life. Early intervention significantly improves outcomes, so it’s important to seek help as soon as symptoms begin to impact daily functioning.
If you’re experiencing symptoms of agoraphobia, remember that effective treatments are available through the NHS. Contact your GP or self-refer to local IAPT services to begin your journey toward recovery. With proper support, you can overcome the limitations imposed by agoraphobia and return to living a full, active life.\n\n
Related Articles

Anxiety Attack Symptoms: How to Recognise and Respond
Learn to recognise anxiety attack symptoms quickly. Understand what's happening in your body and how to respond with confidence.

Anxiety Attack vs Panic Attack: What’s the Difference?
Anxiety attack vs panic attack - what's the difference? Understand the key distinctions so you can respond effectively in the moment.

Chronic Anxiety: When Anxiety Won’t Go Away
When anxiety won't go away, it can feel overwhelming. Understand chronic anxiety and discover strategies to break the long-term cycle.