Treatment options for post-traumatic stress disorder (PTSD): Effective interventions for recovery
Last updated:
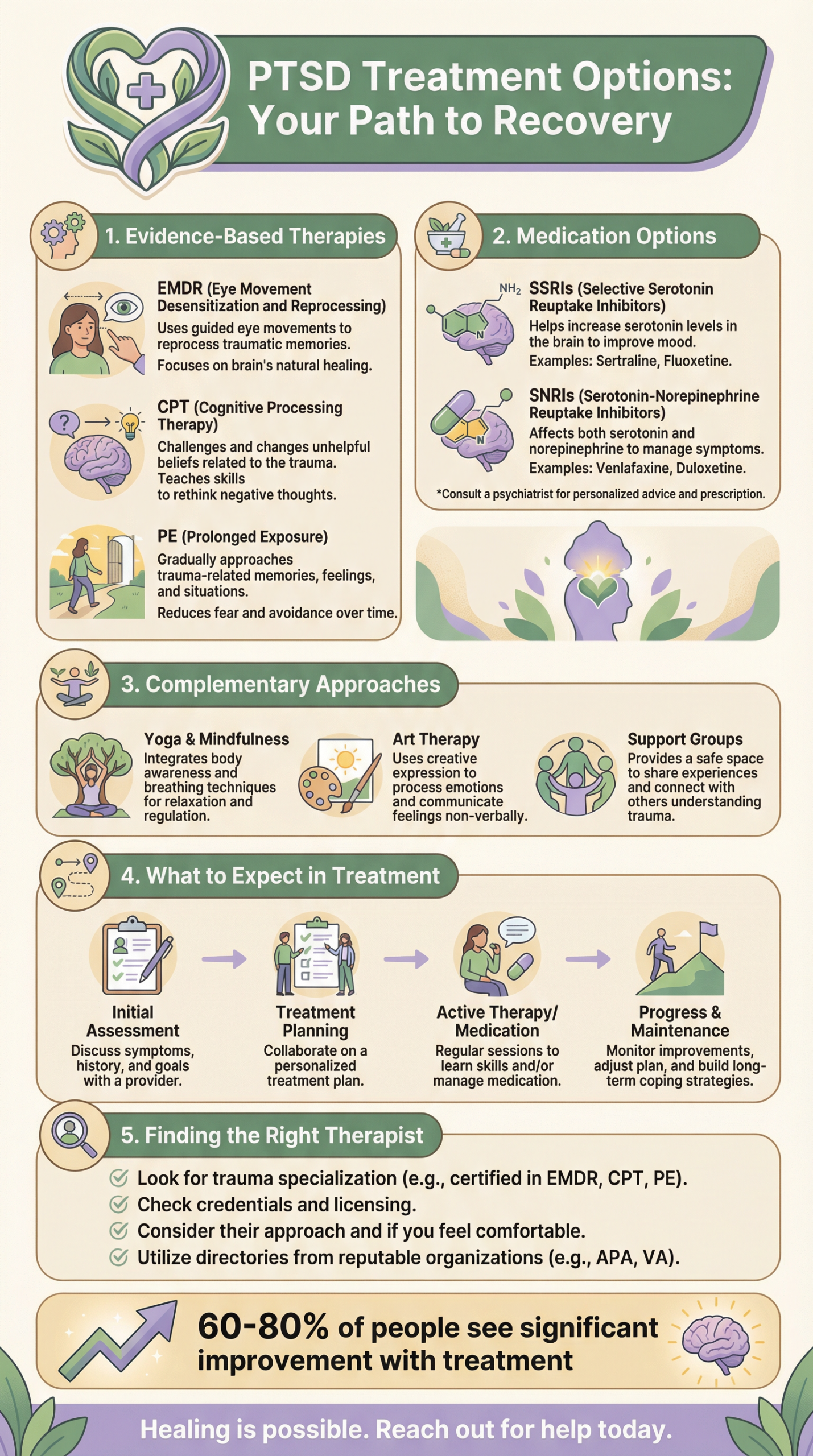
Post-traumatic stress disorder (PTSD) affects many people who have experienced traumatic events. It can cause distressing symptoms that impact daily life. Fortunately, there are several effective treatment options for PTSD. These include talking therapies, medicines, and other supportive approaches.
The main treatments for PTSD are talking therapies and medication. Talking therapies help people process traumatic memories and develop coping skills. Common types include cognitive behavioural therapy (CBT) and eye movement desensitisation and reprocessing (EMDR). Meanwhile, medicines like antidepressants may also be prescribed to help manage symptoms. Treatment plans are tailored to each person’s needs. A combination of therapies often works best. With proper care, many people see significant improvement in their PTSD symptoms and quality of life. Early treatment can help prevent long-term difficulties. Key Takeaways
PTSD is treatable with therapies and medicines tailored to individual needs Talking therapies like CBT help process trauma and develop coping skills Early treatment of PTSD symptoms can prevent long-term mental health issues
Understanding PTSD
Post-traumatic stress disorder (PTSD) is a complex mental health condition that can develop after experiencing or witnessing traumatic events. It affects people differently and can have a significant impact on daily life. Identifying PTSD Symptoms PTSD symptoms can vary in severity and duration. Common signs include intrusive memories and nightmares related to the trauma. People may also experience flashbacks, feeling as if the event is happening again. Avoidance is another key symptom. Those with PTSD often try to avoid thoughts, feelings, or places that remind them of the trauma. This can lead to isolation and withdrawal from activities they once enjoyed. Meanwhile, heightened arousal is also common. This may manifest as:
Irritability or angry outbursts Difficulty concentrating Sleep problems Being easily startled
Negative changes in thoughts and mood are frequent. People might struggle with feelings of guilt, shame, or a distorted sense of self-blame. Factors Leading to Trauma Various events can trigger PTSD. Traumatic experiences often involve threats to life or safety, but any situation that leaves one feeling overwhelmed and helpless can potentially cause PTSD. Common causes include:
Physical or sexual assault Serious accidents Natural disasters Combat exposure Childhood abuse
Not everyone who experiences trauma develops PTSD. Risk factors that increase the likelihood include:
Previous traumatic experiences Existing mental health conditions Lack of social support High levels of stress
The severity and duration of the trauma can also influence the development of PTSD. Prolonged or repeated exposure to traumatic events may increase the risk. Diagnostic Process
Diagnosing post-traumatic stress disorder involves a thorough assessment by mental health professionals using specific criteria. The process aims to accurately identify PTSD symptoms and rule out other conditions. Professional Assessment Mental health experts, such as psychiatrists or psychologists, conduct PTSD assessments. They use clinical interviews and standardised questionnaires to gather information about the patient’s symptoms and experiences. The professional will ask about the traumatic event and how it has affected the person’s life. They may inquire about nightmares, flashbacks, avoidance behaviours, and changes in mood or thinking. Physical exams might be done to check for medical issues that could be causing symptoms. This helps ensure a comprehensive evaluation of the patient’s health. Formal Diagnosis Criteria Mental health professionals use clinical practice guidelines to diagnose PTSD. These guidelines outline specific criteria that must be met for a formal diagnosis. The criteria typically include:

Exposure to a traumatic event Intrusive symptoms (e.g., flashbacks, nightmares) Avoidance of trauma-related stimuli Negative changes in thoughts and mood Changes in arousal and reactivity
Symptoms must persist for more than a month and cause significant distress or impairment in daily life. The professional will also consider the duration of symptoms and their impact on the person’s functioning. It’s important to note that PTSD symptoms can vary among individuals. A thorough assessment helps ensure an accurate diagnosis and appropriate treatment plan. Pharmacological Interventions
Medication can play an important role in treating PTSD symptoms. Several types of drugs have shown effectiveness, with antidepressants being the most commonly prescribed. Antidepressants and SSRIs Selective serotonin reuptake inhibitors (SSRIs) are the primary pharmacological treatment for PTSD. These medicines work by increasing serotonin levels in the brain, which can help improve mood and reduce anxiety. The most effective SSRIs for PTSD include:
Fluoxetine Paroxetine Sertraline
These medications have demonstrated success in reducing PTSD symptoms like flashbacks, nightmares, and hyperarousal. Meanwhile, venlafaxine, a serotonin-norepinephrine reuptake inhibitor (SNRI), has also shown promise in treating PTSD. It’s important to note that medication effects can take several weeks to become noticeable. Patients should work closely with their healthcare provider to find the right dosage and monitor for side effects. Other Medications While antidepressants are the first-line pharmacological treatment for PTSD, other medications may be prescribed in certain cases. Antipsychotics like risperidone, quetiapine, and olanzapine might be considered for patients who don’t respond well to SSRIs. Prazosin, originally developed to treat high blood pressure, has shown effectiveness in reducing PTSD-related nightmares. However, benzodiazepines are generally not recommended for PTSD due to potential for dependency and other risks. It’s crucial to remember that medication should typically be used in conjunction with psychotherapy for optimal results. The choice of medication depends on individual symptoms, medical history, and potential side effects. Psychotherapeutic Treatments
Several effective psychotherapeutic approaches can help people recover from PTSD. These treatments focus on processing traumatic memories, managing symptoms, and developing coping skills. Cognitive-Behavioural Therapies Cognitive-behavioural therapy (CBT) is a widely used and effective treatment for PTSD. It helps patients identify and change negative thought patterns and behaviours related to their trauma. Two specific types of CBT for PTSD are:
Cognitive Processing Therapy (CPT): This approach helps patients examine and modify unhelpful beliefs about their traumatic experience.
Trauma-Focused CBT: This therapy is particularly useful for children and adolescents with PTSD. It involves gradual exposure to trauma reminders and learning coping strategies.
CBT typically lasts 12-16 weeks and may include homework assignments to practise new skills between sessions. EMDR and Exposure Therapies Eye Movement Desensitisation and Reprocessing (EMDR) is a unique therapy that combines exposure to traumatic memories with guided eye movements. This approach aims to help the brain process traumatic memories more effectively. Meanwhile, exposure therapies include:
Prolonged Exposure: Patients gradually confront trauma-related memories, feelings, and situations they’ve been avoiding.
Virtual Reality Exposure: Using computer-generated environments to simulate traumatic experiences in a controlled setting.
These therapies typically last 8-15 sessions and can be highly effective in reducing PTSD symptoms. Additional Psychotherapeutic Approaches Other helpful therapies for PTSD include:

Narrative Exposure Therapy: This approach involves creating a chronological narrative of the patient’s life, including traumatic events.
Group therapy: Sharing experiences with others who have PTSD can provide support and reduce feelings of isolation.
Brief Eclectic Psychotherapy: This combines elements of cognitive-behavioural and psychodynamic therapies.
These treatments may be used alone or in combination with other therapies, depending on the individual’s needs and preferences. Complementary Strategies
Complementary approaches can play a vital role in PTSD treatment. These methods work alongside traditional therapies to support recovery and improve overall wellbeing. Exercise and Lifestyle Changes Regular physical activity can help manage PTSD symptoms. Exercise releases endorphins, which boost mood and reduce stress. A consistent exercise routine may include:
Jogging or brisk walking Swimming Yoga or tai chi Team sports
Healthy lifestyle habits also aid recovery. Proper sleep, a balanced diet, and limiting alcohol can make a big difference. Some find relaxation techniques like deep breathing or meditation helpful. Watchful waiting or active monitoring may be suitable for mild cases. This involves keeping track of symptoms without starting formal treatment right away. Peer Support and Group Therapy Peer support groups offer a safe space for individuals with PTSD to share experiences. These groups can reduce feelings of isolation and provide practical coping tips. Benefits of peer support include:
Shared understanding Emotional support Learning from others’ experiences
Group therapy, led by mental health specialists, combines peer support with professional guidance. It can be a cost-effective way to receive treatment and build a support network. For some, a mix of individual therapy and group sessions works best. Professional help remains crucial, especially for severe PTSD. Specific Considerations
PTSD treatment requires tailored approaches for different groups and conditions. Children and complex cases need specialised care and interventions. PTSD in Children and Adolescents Children and young people with PTSD may need adapted treatments. Trauma-focused cognitive behavioural therapy is often recommended. This helps kids process traumatic memories safely. Play therapy can be useful for younger children. It lets them express feelings through play. Family involvement is crucial for supporting recovery. School-based interventions may help. These can include counselling and teacher training. The goal is to create a supportive environment. Complex PTSD and Comorbid Conditions Complex PTSD often requires longer, more intensive treatment. It may involve a phased approach, with the first phase focusing on safety and stabilisation. Comorbid conditions like anxiety or bipolar disorder need addressing. Integrated treatment plans work best, as these tackle both PTSD and other issues simultaneously. Dialectical behaviour therapy can help manage emotions. It’s useful for those with complex trauma histories. Refugees and asylum seekers may need culturally sensitive care. Language support and understanding of their experiences are vital. Best Practices for Management
Treatment for PTSD often involves a combination of approaches. Talking therapies are a key component. Cognitive behavioural therapy (CBT) is particularly effective. Eye movement desensitisation and reprocessing (EMDR) is another useful technique. It helps patients process traumatic memories through guided eye movements. Medication can play a role in managing symptoms. Selective serotonin reuptake inhibitors (SSRIs) are commonly prescribed for PTSD and associated depression. Sleep problems are common in PTSD. Establishing good sleep hygiene and using relaxation techniques can help combat insomnia. Regular exercise and mindfulness practices can aid in stress reduction and overall well-being. It’s crucial to address co-occurring conditions like depression. Integrated treatment approaches yield better outcomes. Support groups can provide valuable peer support and reduce feelings of isolation. Avoiding alcohol and drugs is important, as substance use can worsen PTSD symptoms. Patient education about PTSD and its treatment is vital. Understanding the condition helps patients engage more effectively in their recovery. Regular follow-ups with healthcare providers allow for treatment adjustments as needed. This ensures the management plan remains effective over time. Frequently Asked Questions
PTSD treatment involves various approaches tailored to each person’s needs. Therapy, medication, and support networks all play key roles in managing symptoms and promoting recovery. What therapeutic approaches are recommended for managing PTSD symptoms? Talking therapies are the primary treatment for PTSD. Trauma-focused cognitive behavioural therapy (TF-CBT) is often used. This approach helps people process traumatic memories and change unhelpful thought patterns. Eye movement desensitisation and reprocessing (EMDR) is another effective therapy. It involves recalling traumatic events while following a therapist’s hand movements. This can help the brain process memories differently. How effective are SSRIs and other medications in treating PTSD? Selective serotonin reuptake inhibitors (SSRIs) are commonly prescribed for PTSD. They can help reduce symptoms like anxiety and depression. Other medications may be used to address specific symptoms, such as sleep problems. Drug treatments are often combined with therapy for best results. The effectiveness varies from person to person, and regular review is important. What novel treatments are emerging for PTSD and how do they work? New treatments for PTSD are being researched. Virtual reality exposure therapy is showing promise. It allows people to confront traumatic situations in a controlled, safe environment. Body-based therapies are gaining attention. These approaches focus on how trauma affects the body and aim to help people feel grounded. Could you explain the best practices for addressing trauma in therapy? Best practices for trauma therapy include creating a safe, trusting environment. Therapists should work at a pace comfortable for the client. Gradual exposure to traumatic memories is often used. Therapists may teach coping skills before delving into traumatic experiences. This helps clients manage distress during treatment. What role does a support network play in the recovery from PTSD? A strong support network is crucial for PTSD recovery. Family and friends can provide emotional support and practical help. Support groups allow people to connect with others who have similar experiences. Social support can reduce feelings of isolation and help maintain progress made in treatment. How does one initially approach treatment for post-traumatic stress disorder? The first step in PTSD treatment is often speaking to a GP. They can assess symptoms and refer to a mental health specialist if needed. Early intervention can improve outcomes. It’s important to find a therapist experienced in treating trauma. Treatment options should be discussed to find the best approach for each individual.
Related Articles

Anxiety Attack Symptoms: How to Recognise and Respond
Learn to recognise anxiety attack symptoms quickly. Understand what's happening in your body and how to respond with confidence.

Anxiety Attack vs Panic Attack: What’s the Difference?
Anxiety attack vs panic attack - what's the difference? Understand the key distinctions so you can respond effectively in the moment.

Chronic Anxiety: When Anxiety Won’t Go Away
When anxiety won't go away, it can feel overwhelming. Understand chronic anxiety and discover strategies to break the long-term cycle.