
Chronic Anxiety: When Anxiety Won’t Go Away
Last updated:
What Is Chronic Anxiety?
Chronic anxiety describes a state of persistent, ongoing anxiety that does not resolve on its own and continues over an extended period. While everyone experiences anxiety from time to time — before an exam, a job interview or a difficult conversation — chronic anxiety is different. It lingers. It is there when you wake up in the morning and when you go to bed at night. It may fluctuate in intensity, but it rarely disappears entirely.
Chronic anxiety is not a formal diagnostic category in the way that generalised anxiety disorder (GAD), panic disorder or social anxiety disorder are. Rather, it is a descriptive term that captures the experience of living with anxiety that has become a seemingly permanent feature of your life. Many people with chronic anxiety meet the criteria for GAD, while others may have a less clearly defined pattern of persistent worry and tension.
If you have been living with anxiety for so long that it feels like part of who you are, it is important to know that this does not mean it has to stay that way. Chronic anxiety can be treated, even if previous attempts have not fully succeeded. New approaches, different therapies or a fresh perspective can make a real difference.
How Chronic Anxiety Differs from Normal Anxiety
Normal anxiety is a functional emotion. It alerts us to potential threats, motivates us to prepare for challenges and keeps us safe. It is proportionate, temporary and tied to specific situations. Once the situation resolves, the anxiety fades.
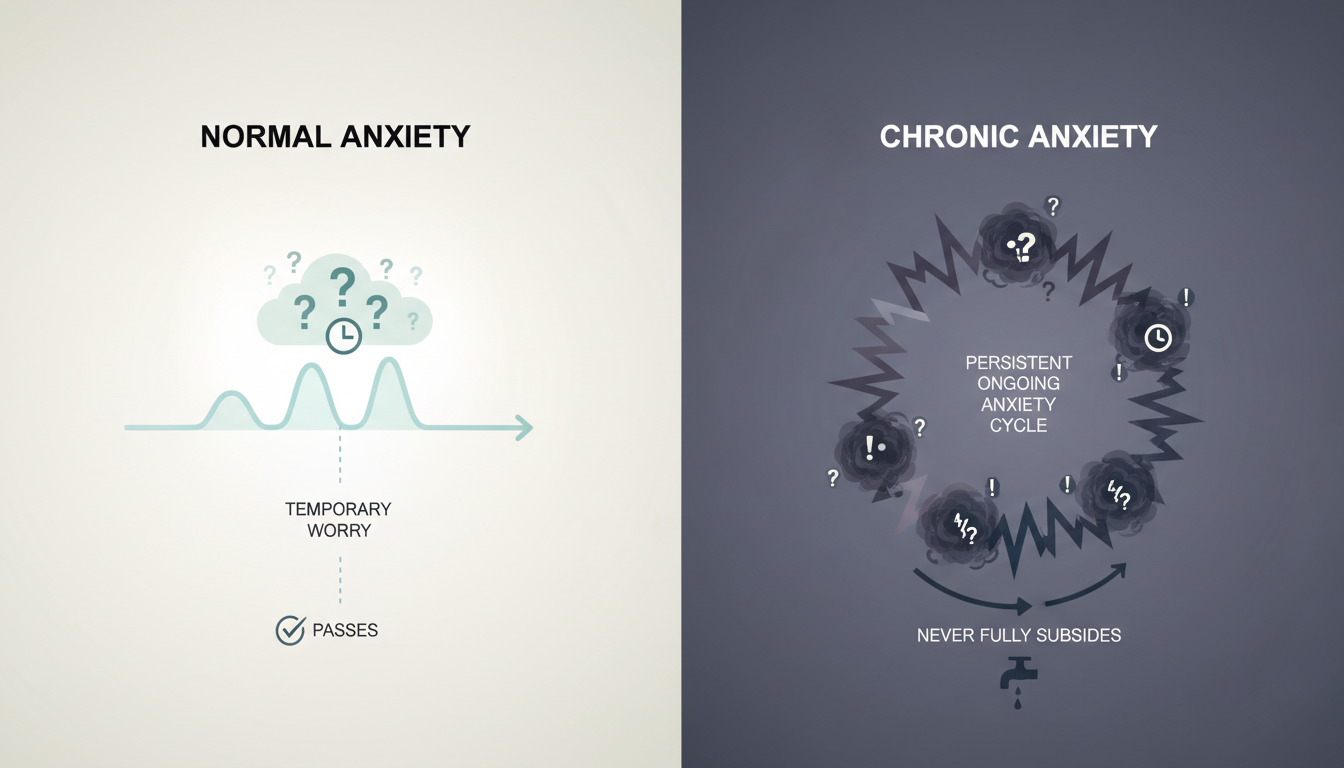
Chronic anxiety, by contrast, has several distinguishing features:
- It is persistent: It continues even when there is no specific threat or stressor, or it moves rapidly from one worry to another.
- It is disproportionate: The level of anxiety is out of proportion to the actual risk or problem.
- It is pervasive: It affects multiple areas of life — work, relationships, health, finances, the future.
- It is resistant: It does not respond to simple reassurance, logical reasoning or the resolution of individual problems.
- It has physical consequences: Long-term activation of the stress response takes a toll on the body.
Symptoms of Chronic Anxiety
The symptoms of chronic anxiety are similar to those of other anxiety disorders but are characterised by their persistence and the cumulative toll they take over time.
Psychological Symptoms
- A constant undercurrent of worry or unease
- Difficulty relaxing or “switching off”
- Feeling on edge, restless or keyed up much of the time
- Irritability and a short temper
- Difficulty concentrating or making decisions
- A sense of dread about the future
- Feeling overwhelmed by everyday tasks
- Low mood and loss of enjoyment in activities you used to find pleasurable
Physical Symptoms
- Chronic muscle tension, particularly in the neck, shoulders, jaw and back
- Persistent fatigue and exhaustion
- Sleep difficulties — trouble falling asleep, staying asleep or waking feeling unrested
- Digestive problems including irritable bowel syndrome (IBS), bloating or nausea
- Frequent headaches or migraines
- Heart palpitations or a feeling of tightness in the chest
- Weakened immune function — catching colds and infections more often
- Changes in appetite (eating more or less than usual)
The Physical Health Impact of Chronic Anxiety
When anxiety persists over a long period, the body’s stress response system remains chronically activated. This has well-documented effects on physical health that deserve attention:
Cardiovascular Health
Chronic anxiety is associated with increased risk of cardiovascular problems. Persistent elevation of stress hormones such as cortisol and adrenaline can raise blood pressure, increase heart rate and promote inflammation in the blood vessels. Research published in the British Medical Journal has linked chronic anxiety with a modestly increased risk of coronary heart disease.
Digestive Health
The gut and the brain are intimately connected through the gut-brain axis. Chronic anxiety frequently manifests as digestive problems, and there is a strong association between anxiety disorders and irritable bowel syndrome (IBS). The NHS acknowledges that stress and anxiety are among the most common triggers for IBS symptoms.
Immune Function
Prolonged stress and anxiety can suppress immune function, making you more susceptible to infections and slowing wound healing. This is one reason why people under chronic stress often find they are ill more frequently.
Pain
Chronic anxiety can lower your pain threshold and increase sensitivity to pain. It is also closely linked with chronic pain conditions such as fibromyalgia and tension-type headaches.
Why Does Anxiety Become Chronic?
Several factors can contribute to anxiety becoming a long-term condition:
Avoidance
Avoidance is one of the most powerful maintaining factors for any anxiety condition. When you avoid the things that make you anxious, you get short-term relief but long-term perpetuation of the problem. You never get the opportunity to learn that you can cope, and the feared situation becomes even more daunting over time.
Unhelpful Thinking Patterns
Over years, anxious thinking patterns can become deeply ingrained. Catastrophising, overestimating danger, underestimating your ability to cope, and intolerance of uncertainty can become habitual ways of processing the world that feel automatic and unchangeable.
Life Circumstances
Ongoing stressors such as financial difficulty, caring responsibilities, an unsupportive work environment, relationship problems or chronic illness can keep anxiety at a high level. Addressing anxiety solely through psychological techniques while ignoring genuine external stressors is unlikely to be fully effective.
Biological Factors
Some people may have a biological predisposition to anxiety that makes it more likely to persist. Differences in brain chemistry, nervous system sensitivity and genetic factors can all contribute to a lower threshold for anxiety activation.
Previous Trauma
Unresolved trauma, whether from childhood or adulthood, can be a significant driver of chronic anxiety. If trauma has not been addressed, anxiety may persist despite treatment targeting the anxiety itself.
Treatment Approaches for Chronic Anxiety
Treating chronic anxiety often requires a more comprehensive and sustained approach than treating a newly developed anxiety condition.
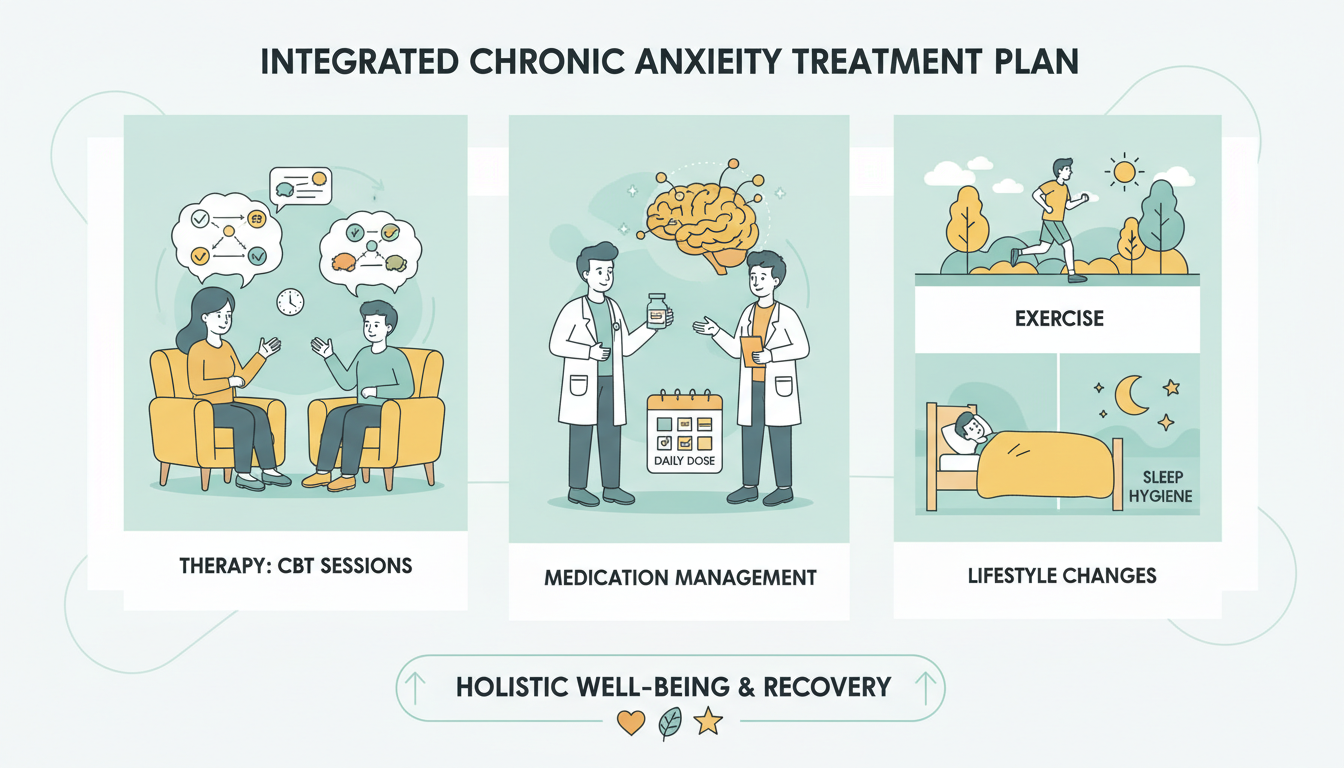
Cognitive Behavioural Therapy (CBT)
CBT remains the most evidence-based psychological treatment and is recommended by NICE for anxiety disorders. For chronic anxiety, it may be helpful to seek a longer or more intensive course of CBT than the standard 6-12 sessions, particularly if previous shorter courses have not been sufficient.
Acceptance and Commitment Therapy (ACT)
ACT can be particularly valuable for chronic anxiety. Rather than focusing primarily on reducing anxiety, ACT helps you develop a different relationship with anxious thoughts and feelings — learning to observe them without being controlled by them. It emphasises living a valued and meaningful life even in the presence of anxiety, which can be a more realistic and sustainable goal for long-term sufferers.
Mindfulness-Based Approaches
Mindfulness-based cognitive therapy (MBCT) and mindfulness-based stress reduction (MBSR) have a growing evidence base for anxiety. These programmes teach you to relate to your thoughts and emotions with greater awareness and less reactivity. The NHS mental health charity Mind highlights mindfulness as a helpful approach for managing ongoing anxiety.
Medication
For chronic anxiety, longer-term medication may be appropriate. NICE recommends SSRIs as first-line medication for anxiety disorders. If you are taking medication for chronic anxiety, it is generally advisable to continue for at least 12 months after symptoms improve, and any reduction should be gradual and supervised by your GP.
Addressing Underlying Factors
If chronic anxiety is linked to unresolved trauma, trauma-focused therapies such as eye movement desensitisation and reprocessing (EMDR) or trauma-focused CBT may be beneficial. If there are significant life circumstances maintaining the anxiety, practical support (such as debt advice, relationship counselling or occupational health input) may be an important part of the treatment plan.
Lifestyle Strategies for Long-Term Management
- Regular physical activity: Exercise is one of the most consistently supported strategies for reducing anxiety. Aim for at least 150 minutes of moderate-intensity activity per week, as recommended by the NHS.
- Sleep hygiene: Prioritise consistent sleep patterns, limit screen time before bed and create a calming bedtime routine.
- Nutrition: A balanced diet supports both physical and mental health. Reduce caffeine, which can worsen anxiety, and maintain regular mealtimes.
- Social connection: Maintain relationships and social activities, even when anxiety makes it tempting to withdraw.
- Relaxation practices: Regular relaxation techniques such as progressive muscle relaxation, deep breathing or yoga can help lower your baseline anxiety level over time.
- Limit alcohol: While alcohol may temporarily ease anxiety, it worsens it in the longer term and can interfere with sleep, mood and medication.
- Structure and routine: A predictable daily routine can provide a sense of stability and control that helps manage chronic anxiety.
When to Seek Help
You should seek professional support if:
- Anxiety has been a persistent feature of your life for months or years
- You feel unable to enjoy life or function as you would like to because of anxiety
- Physical symptoms of anxiety (tension, fatigue, digestive problems, sleep difficulties) are affecting your health
- Previous treatment has not been effective, and you wonder if a different approach might help
- You are using alcohol, drugs or other unhealthy strategies to manage your anxiety
- You are experiencing low mood, hopelessness or thoughts of self-harm alongside anxiety
If you have tried treatment before without success, do not give up. It may be that a different type of therapy, a different therapist, the addition of medication, or addressing underlying factors such as trauma or life circumstances could make the difference.
Where to get help in the UK:
- NHS Talking Therapies: Self-refer for free therapy at nhs.uk.
- Your GP: Can review medication, refer to specialist mental health services and coordinate your care.
- Mind: Comprehensive information and local support services. Infoline: 0300 123 3393.
- Anxiety UK: Dedicated anxiety support, including access to therapy. Helpline: 03444 775 774.
- Samaritans: 24/7 emotional support on 116 123.
- Shout: Free 24/7 text support. Text SHOUT to 85258.
Related Articles

Anxiety Attack Symptoms: How to Recognise and Respond
Learn to recognise anxiety attack symptoms quickly. Understand what's happening in your body and how to respond with confidence.

Anxiety Attack vs Panic Attack: What’s the Difference?
Anxiety attack vs panic attack - what's the difference? Understand the key distinctions so you can respond effectively in the moment.

CBT Techniques Social Anxiety UK: Effective NHS-Approved Methods for Self-Help and Recovery
Discover proven CBT techniques social anxiety UK specialists use, access NHS talking therapies social anxiety services, and learn effective social anxiety self help UK strategies for lasting...