
CBT for Anxiety: How It Works, Techniques and How to Access It
Last updated:
What Is CBT?
Cognitive behavioural therapy (CBT) is a structured, evidence-based talking therapy that focuses on the relationship between your thoughts, feelings and behaviours. Originally developed by the American psychiatrist Dr Aaron T. Beck in the 1960s, CBT has become the most widely researched and recommended psychological treatment for anxiety disorders worldwide.

Unlike some other forms of therapy, CBT does not spend a great deal of time exploring your childhood or unconscious motivations. Instead, it is firmly rooted in the present. A CBT therapist will work with you to identify specific patterns of thinking and behaviour that are keeping your anxiety going, and then help you develop practical strategies to change them.
How CBT Differs from Other Therapies
If you have looked into therapy options, you may have come across several different approaches. Understanding how CBT compares can help you decide whether it is right for you.
- CBT vs counselling: Person-centred counselling provides a supportive space to talk through your feelings, but it tends to be less structured and does not typically teach specific techniques. CBT is more directive and goal-oriented, with a clear focus on changing thought and behaviour patterns.
- CBT vs psychodynamic therapy: Psychodynamic therapy explores how past experiences, particularly from childhood, shape your current emotional life. CBT acknowledges the past but focuses primarily on present-day thinking patterns and practical solutions.
- CBT vs EMDR: Eye movement desensitisation and reprocessing (EMDR) is primarily used for trauma and post-traumatic stress disorder (PTSD). While both EMDR and CBT are recommended by NICE, they work through different mechanisms.
- CBT vs mindfulness-based cognitive therapy (MBCT): MBCT combines CBT principles with mindfulness meditation. It is particularly recommended for preventing relapse in depression, while standard CBT is the first-line recommendation for most anxiety disorders.
The key advantage of CBT is that it gives you a toolkit of skills you can continue to use long after therapy ends. Research consistently shows that the benefits of CBT tend to be maintained over time, partly because you learn to become your own therapist.
How Does CBT Work for Anxiety?
At the heart of CBT is a simple but powerful idea: it is not events themselves that cause us distress, but the meaning we attach to them. When you are anxious, your mind tends to interpret situations as more dangerous or threatening than they actually are. CBT helps you recognise these patterns and develop more balanced, realistic ways of thinking.
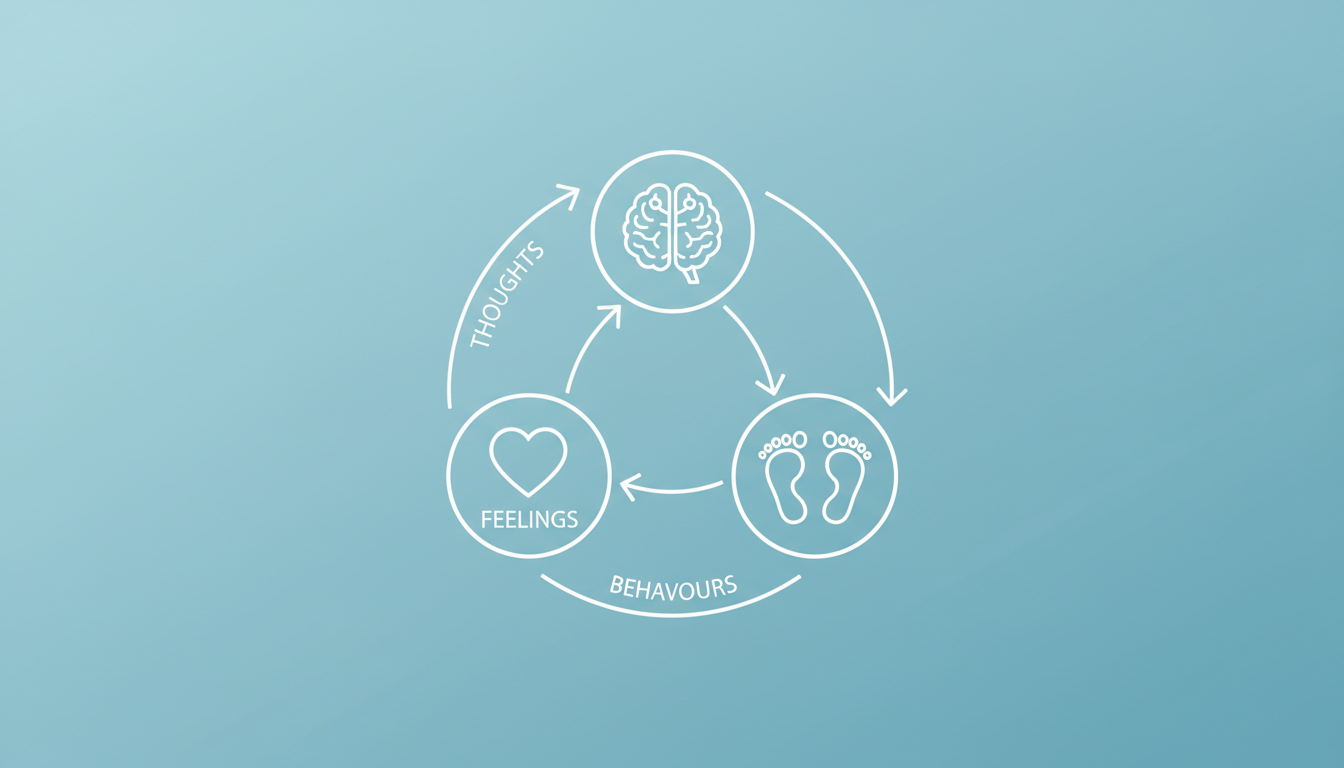
The Cognitive Model: Thoughts, Feelings and Behaviours
CBT is built on what therapists call the cognitive model — the understanding that thoughts, feelings, physical sensations and behaviours are all interconnected, and that changing one can influence the others.
Here is how the cycle typically works with anxiety:
- Situation: You are invited to a social gathering where you will not know many people.
- Thought (cognition): “Everyone will think I’m boring. I’ll have nothing to say and people will judge me.”
- Feeling (emotion): Intense anxiety, dread, self-consciousness.
- Physical sensation: Stomach churning, heart racing, sweating, chest tightness.
- Behaviour: You make an excuse and decline the invitation (avoidance).
The problem with avoidance is that while it brings temporary relief, it actually reinforces the anxiety. You never get the chance to discover that the feared outcome probably would not have happened. Over time, the avoidance tends to spread — you might start declining more and more invitations, and your world gradually shrinks.
CBT breaks into this cycle at multiple points. You learn to:
- Identify the negative automatic thoughts that trigger your anxiety
- Evaluate whether those thoughts are accurate or whether they are distorted by anxiety
- Test your fearful predictions through real-world experiments
- Gradually face situations you have been avoiding, building confidence step by step
- Develop new, healthier responses to anxiety-provoking situations
Common Thinking Errors in Anxiety
CBT identifies several types of thinking errors (sometimes called cognitive distortions) that are particularly common in anxiety:
- Catastrophising: Jumping to the worst possible outcome. “If I make a mistake at work, I’ll be sacked.”
- Mind reading: Assuming you know what others are thinking. “Everyone at the meeting could see how nervous I was.”
- Fortune telling: Predicting the future negatively. “The presentation is going to go terribly.”
- Black-and-white thinking: Seeing things in all-or-nothing terms. “If I can’t do it perfectly, there’s no point trying.”
- Overestimating threat: Believing that something dangerous is more likely than it actually is. “If I drive on the motorway, I’ll definitely crash.”
- Underestimating coping: Believing you cannot handle difficult situations. “I won’t be able to cope if I have a panic attack in public.”
Recognising these patterns is the first step towards changing them. Most people find that once they become aware of their thinking errors, they start to notice them more quickly and can challenge them more effectively.
Is CBT Effective for Anxiety? What the Research Says
CBT is one of the most extensively researched psychological treatments in existence, and the evidence for its effectiveness in treating anxiety disorders is strong.
NICE Recommendations
The National Institute for Health and Care Excellence (NICE), which sets the standard for evidence-based healthcare in England and Wales, recommends CBT as a first-line treatment for the following anxiety disorders:
- Generalised anxiety disorder (GAD): NICE guideline CG113 recommends CBT as the psychological treatment of choice, with either individual or group-based CBT offered depending on patient preference and availability.
- Social anxiety disorder: NICE guideline CG159 specifically recommends individual CBT based on the Clark and Wells model as the first-line treatment, noting that it should be offered before medication.
- Panic disorder: NICE recommends CBT as the psychological treatment with the strongest evidence base, typically delivered over 7 to 14 sessions.
- Specific phobias: NICE recommends exposure-based CBT techniques as the treatment of choice.
- Obsessive-compulsive disorder (OCD): NICE recommends CBT that includes exposure and response prevention (ERP) as a first-line treatment.
- Post-traumatic stress disorder (PTSD): Trauma-focused CBT is recommended by NICE alongside EMDR.
What the Research Shows
The evidence base for CBT in anxiety is substantial:
- A major meta-analysis published in the journal Psychological Medicine found that CBT produced large effect sizes for anxiety disorders, with benefits maintained at follow-up assessments.
- Research published in the Cochrane Database of Systematic Reviews confirmed that CBT is significantly more effective than waiting-list controls for generalised anxiety disorder.
- Studies consistently show that approximately 50-60% of people with anxiety disorders achieve clinically significant improvement following a course of CBT.
- The benefits of CBT appear to be long-lasting. Follow-up studies show that most people maintain their gains for at least one to two years after treatment ends, and many continue to improve after therapy finishes.
It is worth noting that CBT does not work for everyone, and that is perfectly normal. If you try CBT and find it is not helpful, other evidence-based treatments are available, including medication, other forms of therapy, or a combination approach.
5 CBT Techniques You Can Try Today
While working with a trained therapist is ideal, there are several core CBT techniques you can begin practising on your own. These techniques form the building blocks of CBT for anxiety and can make a meaningful difference even when used independently.

1. Thought Records: Challenging Negative Thoughts
A thought record is one of the most fundamental CBT tools. It helps you slow down your thinking, examine your anxious thoughts more objectively, and develop more balanced alternatives.
How to do it:
- Step 1: When you notice your anxiety rising, pause and write down the situation. What is happening? Where are you? What triggered the anxiety?
- Step 2: Write down the automatic thought — the first thing that went through your mind. For example: “I’m going to embarrass myself in this meeting.”
- Step 3: Rate how strongly you believe the thought (0-100%) and how intense your anxiety feels (0-100%).
- Step 4: Look for evidence that supports the thought. Be specific and factual.
- Step 5: Now look for evidence against the thought. Have you managed similar situations before? What would you say to a friend who had this thought?
- Step 6: Write a more balanced, realistic thought. For example: “I’ve presented before and it went reasonably well. Even if I stumble over my words, people are unlikely to judge me harshly.”
- Step 7: Re-rate your belief in the original thought and your anxiety level. Most people find both have reduced.
With regular practice, this process becomes quicker and more natural. Many people find they can eventually challenge anxious thoughts in their head, without needing to write them down.
2. Behavioural Experiments: Testing Your Predictions
Behavioural experiments are one of the most powerful techniques in CBT. The idea is simple: rather than just talking about whether your anxious thoughts are accurate, you test them in the real world.
How to do it:
- Step 1: Identify a specific anxious prediction. For example: “If I speak up in the team meeting, people will think I’m stupid.”
- Step 2: Rate how strongly you believe this prediction (0-100%).
- Step 3: Design an experiment to test it. In this case, you might plan to make one comment or ask one question in your next team meeting.
- Step 4: Predict what you think will happen. Be specific: “People will look at me strangely, and no one will respond to what I say.”
- Step 5: Carry out the experiment.
- Step 6: Record what actually happened. Was your prediction accurate? What did you learn?
- Step 7: Re-rate your belief in the original prediction.
Most people find that the feared outcome either does not happen at all or is far less severe than they expected. Over time, these experiments build a body of evidence that helps to weaken anxious beliefs.
3. Exposure Hierarchy: Facing Your Fears Gradually
Avoidance is one of the main factors that keeps anxiety going. Exposure therapy, a core component of CBT, involves gradually and systematically facing the situations you have been avoiding.
How to do it:
- Step 1: Write a list of situations related to your anxiety that you currently avoid or find difficult. Be as specific as possible.
- Step 2: Rate each situation on a scale of 0-100 based on how much anxiety it would cause (this is sometimes called your SUDS — Subjective Units of Distress Scale).
- Step 3: Arrange the situations in order from least to most anxiety-provoking. This is your exposure hierarchy.
- Step 4: Start with the lowest-rated item on your list. Stay in the situation until your anxiety begins to reduce naturally (this usually takes 20-45 minutes).
- Step 5: Repeat the same exposure until the anxiety it causes has reduced significantly (aim for a 50% reduction in your SUDS rating).
- Step 6: Move up to the next item on your hierarchy and repeat the process.
The key principle is that anxiety naturally reduces over time if you stay in the situation rather than escaping. Each successful exposure teaches your brain that the situation is not as dangerous as it believed.
4. Activity Scheduling: Breaking the Avoidance Cycle
When you are anxious, it is natural to withdraw from activities and spend more time avoiding or worrying. Activity scheduling helps you break this pattern by planning meaningful, enjoyable or achievement-oriented activities into your day.
How to do it:
- Step 1: For one week, keep a simple diary of what you do each day and rate each activity for both pleasure (0-10) and achievement (0-10).
- Step 2: Review your diary. You may notice that you are spending a lot of time on activities that bring neither pleasure nor a sense of achievement (such as scrolling on your phone or lying in bed worrying).
- Step 3: Plan your next week in advance, scheduling a balanced mix of:
- Pleasurable activities: Things you enjoy, even if anxiety makes them feel less appealing than usual (meeting a friend, going for a walk, cooking a favourite meal).
- Achievement activities: Tasks that give you a sense of accomplishment (completing a work project, tidying a room, exercising).
- Necessary activities: Everyday tasks that need to be done (shopping, housework, appointments).
- Step 4: Treat your schedule like an appointment with yourself. Try to follow it even when you do not feel like it — anxiety often reduces once you actually start the activity.
- Step 5: Review at the end of the week. Did doing more activities improve your mood and reduce your anxiety?
5. Relaxation Training: Calming the Physical Symptoms
Anxiety produces very real physical symptoms — racing heart, muscle tension, shallow breathing, stomach churning. Relaxation techniques help to activate the parasympathetic nervous system (your body’s natural calming system) and reduce these physical symptoms.
Diaphragmatic breathing:
- Sit or lie comfortably. Place one hand on your chest and one on your stomach.
- Breathe in slowly through your nose for 4 counts, allowing your stomach (not your chest) to rise.
- Hold for 2 counts.
- Breathe out slowly through your mouth for 6 counts.
- Repeat for 5-10 minutes. Practise twice daily, not just when you are anxious.
Progressive muscle relaxation (PMR):
- Find a quiet, comfortable place and close your eyes.
- Starting with your feet, tense each muscle group for 5 seconds, then release for 10 seconds.
- Work your way up through your calves, thighs, stomach, chest, arms, shoulders, neck and face.
- Notice the contrast between tension and relaxation.
- The full exercise takes about 15-20 minutes.
Regular practice of relaxation techniques is important. The more you practise when you are calm, the more effective they will be when you are anxious.
How to Practise CBT at Home
While professional therapy is the gold standard, there is good evidence that self-guided CBT can also be effective, particularly for mild to moderate anxiety. NICE recognises self-help CBT as a valid treatment option and recommends it as a first step for many anxiety disorders.

Self-Help Books
Several excellent CBT self-help books are available, many of which are recommended by NHS Talking Therapies services:
- Overcoming Anxiety by Helen Kennerley: A comprehensive self-help guide based on CBT principles, widely recommended by UK therapists.
- Mind Over Mood by Dennis Greenberger and Christine Padesky: A structured workbook that guides you through CBT techniques step by step, with exercises and worksheets.
- The Feeling Good Handbook by David D. Burns: One of the original CBT self-help books, with practical exercises for anxiety and depression.
- Overcoming Social Anxiety and Shyness by Gillian Butler: Specifically designed for social anxiety, part of the well-regarded Overcoming series.
CBT Worksheets
Free CBT worksheets are available from several reputable sources. These typically include thought records, exposure hierarchy templates, behavioural experiment logs and activity schedules. Your NHS Talking Therapies service may also provide worksheets as part of guided self-help.
CBT Apps
Several digital CBT programmes and apps have evidence supporting their use:
- SilverCloud: An online CBT programme that is available free on the NHS in many areas. It provides structured modules with therapist support and has a strong evidence base.
- Wysa: An AI-powered mental health app that uses CBT-based techniques. Available on iOS and Android with both free and premium options.
- Woebot: A chatbot-style app that delivers CBT-based conversations and mood tracking. Research published in the Journal of Medical Internet Research supports its effectiveness.
- Feeling Good (NHS-approved app): Available through some NHS Talking Therapies services, providing structured CBT content.
Self-help CBT works best when you treat it like a course rather than casual reading. Set aside regular time each week, complete the exercises, and give it at least 6 to 8 weeks before evaluating whether it is helping.
How to Access CBT in the UK
If you would like to try CBT with a professional therapist, there are several routes available in the UK.

NHS Talking Therapies (Free)
The NHS Talking Therapies programme (formerly known as IAPT — Improving Access to Psychological Therapies) is the main route to free CBT on the NHS in England. Here is what you need to know:
- Self-referral: In most areas of England, you can refer yourself directly to your local Talking Therapies service without needing a GP referral. Visit the NHS website and search for “NHS Talking Therapies” to find your local service.
- What to expect: You will typically have an initial assessment by telephone, during which a therapist will ask about your symptoms and difficulties. Based on this assessment, you may be offered guided self-help (step 2) or individual CBT sessions (step 3).
- Waiting times: The NHS target is for 75% of people to start treatment within 6 weeks of referral, and 95% within 18 weeks. In practice, waiting times vary significantly depending on your area. Some services have waits of several months, particularly for individual therapy. Your local service can give you an estimate when you are assessed.
- Format: CBT may be offered face-to-face, by video call, by telephone, or through an online programme. Many services have expanded their remote options since 2020.
- In Scotland, Wales and Northern Ireland: Similar services exist but the referral process may differ. In Scotland, you can access psychological therapies through your GP. In Wales, the NHS offers therapy through Local Primary Mental Health Support Services. In Northern Ireland, therapy is available through the regional health trusts.
Private CBT
If you prefer not to wait for NHS treatment, or if you want more flexibility in choosing your therapist, private CBT is available throughout the UK.
- Finding a therapist: The British Association for Behavioural and Cognitive Psychotherapies (BABCP) maintains a register of accredited CBT therapists. Searching the BABCP register is the best way to find a qualified, accredited private CBT therapist near you or offering online sessions.
- Cost: Private CBT sessions typically cost between £50 and £100 per session, depending on the therapist’s experience, location and whether sessions are conducted in person or online. Sessions in London and the South East tend to be at the higher end of this range.
- Insurance: Some private health insurance policies cover CBT. Check with your provider before starting treatment.
- Frequency: Private CBT is usually offered weekly, with each session lasting 50-60 minutes.
Online CBT Options
Online CBT has grown significantly and can be a flexible, effective option:
- Therapist-led online CBT: Many BABCP-accredited therapists offer sessions by video call, providing the same quality of treatment as face-to-face sessions. Research shows that online CBT is as effective as in-person therapy for most anxiety disorders.
- Computerised CBT (cCBT): Programmes such as SilverCloud deliver structured CBT content online, often with light-touch therapist support via messaging. These are available through some NHS services and privately.
- Charity-provided therapy: Organisations such as Anxiety UK offer CBT sessions at reduced rates for their members, including online options.
What to Expect in CBT Sessions
Knowing what to expect can help reduce any anxiety you might feel about starting therapy. Here is a typical outline of how CBT for anxiety works in practice.
Structure of a Typical Session
CBT sessions tend to follow a consistent structure, which many people find reassuring:
- Check-in (5-10 minutes): Your therapist will ask how your week has been, review any questionnaires (such as the GAD-7 anxiety scale), and set an agenda for the session together.
- Homework review (10-15 minutes): You will discuss the between-session tasks you completed — what went well, what was difficult, and what you learned.
- Main session content (20-30 minutes): This is where the core therapeutic work happens. You might learn a new technique, work through a specific anxious situation, review a thought record, or plan a behavioural experiment.
- Homework setting (5-10 minutes): Your therapist will agree on tasks for you to practise before the next session. Homework is a crucial part of CBT — research shows that people who complete between-session tasks tend to have better outcomes.
- Summary and feedback (5 minutes): You will briefly summarise the key points from the session, and your therapist will ask for feedback on how the session felt.
The Role of Homework
Homework is a central part of CBT, and this is one of the features that makes it different from many other therapies. Your therapist may ask you to:
- Complete thought records when you notice anxiety
- Carry out behavioural experiments between sessions
- Practise exposure exercises from your hierarchy
- Keep a diary of your anxiety levels and triggers
- Read information about your specific type of anxiety
- Practise relaxation techniques daily
The homework is not about doing it perfectly — it is about practising new skills and gathering information that you and your therapist can discuss together. If you find the homework too difficult or too easy, your therapist can adjust it.
Number of Sessions
The number of CBT sessions varies depending on the type and severity of your anxiety:
- Mild to moderate anxiety: Guided self-help programmes typically involve 6 to 8 sessions of support.
- Moderate anxiety: Individual CBT is commonly offered over 8 to 12 sessions.
- Severe or complex anxiety: Treatment may extend to 12 to 20 sessions, particularly for conditions such as OCD or PTSD.
- NICE guidance: For panic disorder, NICE suggests 7 to 14 sessions. For social anxiety, the recommendation is up to 14 sessions of individual CBT. For GAD, the guideline suggests offering a course of individual CBT, typically consisting of 12 to 15 sessions.
Sessions are usually held weekly, and treatment typically lasts between 3 and 5 months. Some therapists may offer fortnightly sessions towards the end of treatment to help you practise independently before finishing.
When to Seek Professional Help
Self-help CBT techniques are valuable, but there are times when professional support is important. Consider seeking help from a therapist or your GP if:
- Anxiety is interfering with your daily life: If anxiety is making it difficult to work, study, maintain relationships, or carry out everyday tasks, professional CBT can help you regain functioning more quickly.
- You are experiencing panic attacks: Recurrent panic attacks can be effectively treated with CBT, and professional guidance is important to ensure the right techniques are used.
- Self-help has not been enough: If you have tried self-help techniques for 6 to 8 weeks without noticeable improvement, it may be time to work with a therapist who can tailor the approach to your specific needs.
- You are avoiding more and more situations: If avoidance is spreading and your world is getting smaller, a therapist can help you develop a structured exposure plan.
- You are experiencing physical symptoms: Persistent physical symptoms such as chest pain, breathlessness or dizziness should be checked by your GP to rule out physical causes, and then addressed with appropriate psychological treatment.
- You are using alcohol or other substances to cope: If you find yourself relying on alcohol, drugs or other substances to manage your anxiety, it is important to seek professional help.
- You are having thoughts of self-harm or suicide: If anxiety is accompanied by thoughts of harming yourself, please reach out for help immediately. Contact the Samaritans on 116 123 (free, 24 hours), text SHOUT to 85258, or call 999 in an emergency.
Seeking professional help is not a sign of failure — it is a practical, sensible step towards recovery. Most people with anxiety disorders respond well to treatment, and the sooner you start, the sooner you can begin to feel better.
UK Resources for Getting Help
- NHS Talking Therapies: Self-refer for free CBT at nhs.uk/talking-therapies
- BABCP therapist register: Find a private accredited CBT therapist at babcp.com
- Anxiety UK: Therapy and support for anxiety — 03444 775 774 — anxietyuk.org.uk
- Mind: Information and support for mental health — 0300 123 3393 — mind.org.uk
- Samaritans: 24-hour emotional support — 116 123 (free) — samaritans.org
- No Panic: Support for panic attacks, phobias and OCD — 0300 772 9844 — nopanic.org.uk
Frequently Asked Questions
How long does CBT take to work for anxiety?
Most people begin to notice some improvement within the first 4 to 6 sessions of CBT, though this varies depending on the type and severity of the anxiety. A full course of CBT typically lasts between 6 and 20 sessions, usually delivered weekly. NICE guidelines suggest that significant improvement is expected by the end of treatment. Some people feel better quickly, while others need the full course to see meaningful change. The key is to practise the techniques consistently between sessions — research shows that people who complete their homework tend to recover more quickly.
Can I do CBT on my own?
Yes, to an extent. Self-guided CBT using books, workbooks, apps or online programmes can be effective for mild to moderate anxiety. NICE recognises self-help CBT as a valid treatment step. However, working with a trained therapist offers several advantages: they can tailor the approach to your specific difficulties, help you overcome obstacles, provide accountability, and address issues that might be difficult to work through alone. If you start with self-help and find it is not sufficient after 6 to 8 weeks, it is worth considering professional support.
Is CBT available free on the NHS?
Yes. In England, you can access free CBT through the NHS Talking Therapies programme. In most areas, you can self-refer directly without needing a GP referral. The service offers both guided self-help and individual CBT sessions. Similar services exist in Scotland, Wales and Northern Ireland, though the referral process may differ. Waiting times vary by area — the NHS target is for treatment to begin within 6 to 18 weeks, but some areas have longer waits. Your local service can give you an estimated waiting time when you are assessed.
What is the difference between CBT and counselling?
CBT and counselling are both talking therapies, but they work quite differently. CBT is structured, goal-oriented and focused on changing specific patterns of thinking and behaviour. Sessions follow a set format, include homework tasks, and therapy has a defined number of sessions. Counselling, particularly person-centred counselling, is less structured and provides a supportive space for you to explore your feelings at your own pace. Both can be helpful, but for anxiety disorders specifically, NICE recommends CBT as the first-line psychological treatment because it has a stronger evidence base.
How many CBT sessions will I need?
The number of sessions depends on the type and severity of your anxiety. As a general guide: guided self-help typically involves 6 to 8 supported sessions; individual CBT for most anxiety disorders is commonly 8 to 15 sessions; more complex conditions such as OCD or PTSD may require 12 to 20 sessions. NICE provides specific guidance for different conditions — for example, 7 to 14 sessions for panic disorder, and up to 14 sessions for social anxiety disorder. Your therapist will discuss the expected number of sessions with you at the start of treatment.
Does CBT work for all types of anxiety?
CBT has a strong evidence base for most types of anxiety, including generalised anxiety disorder, social anxiety disorder, panic disorder, specific phobias, obsessive-compulsive disorder and post-traumatic stress disorder. However, no single treatment works for everyone. Research suggests that approximately 50-60% of people with anxiety disorders achieve clinically significant improvement with CBT. If CBT does not work for you, your therapist or GP can discuss alternative options, which may include different types of therapy, medication, or a combination approach. The important thing is not to give up — there are multiple effective treatments available.
Related Articles

Breathing Exercises for Anxiety: 7 Techniques to Calm Your Mind
Breathing exercises are one of the fastest ways to calm anxiety. Try these 7 techniques and feel the difference in minutes.
Calm Anxiety: The Perfect Evening Routine
Evening Routine to Ease Down Anxiety: A Comprehensive Guide Anxiety has become a common part of modern life, affecting millions worldwide. With the constant demands of work, social...

Coop with Anxiety: Strategies to Overcome and Manage Anxiety
Are you struggling with anxiety and looking for effective strategies to overcome and manage it? Look no further! In this blog post, I’ll be sharing valuable insights and techniques to…